Chronic Kidney Disease: Causes, Symptoms, and Effective Treatment Options
Introduction
Chronic kidney disease (CKD) is a significant and often underestimated health issue affecting millions globally. This condition develops gradually, diminishing the kidneys’ ability to filter waste and excess fluids from the bloodstream effectively. As kidney function declines, harmful toxins can accumulate, resulting in various health problems.
CKD is often referred to as a “silent disease” because many individuals may not notice symptoms during its early stages. By the time clear indicators emerge, the disease could be well-advanced, complicating treatment. Therefore, awareness and early detection are essential.
The increasing incidence of CKD is closely associated with modern lifestyle diseases such as diabetes and hypertension, which are among its primary causes. If not managed properly, CKD can progress to kidney failure, necessitating critical interventions like dialysis or a kidney transplant.
This article will provide comprehensive information on chronic kidney disease—including its causes, warning signs, effective treatment options, and practical lifestyle recommendations. Whether you’re aiming to maintain kidney health or manage an existing issue, this guide will offer useful, dependable, and actionable insights.
3. Stages of Chronic Kidney Disease
Chronic Kidney Disease is categorized into five stages based on kidney function, measured by a test known as the glomerular filtration rate (GFR), which assesses how effectively the kidneys filter wastes from the blood.
Understanding these stages is vital for guiding treatment and lifestyle modifications aimed at slowing disease progression.
Stage 1: Kidney Damage with Normal Function (GFR ≥ 90)
– The kidneys are functioning normally, yet early damage may be present (e.g., protein in urine).
– Symptoms are often absent.
– Typically identified through routine testing.
Key Focus:
Early intervention—manage underlying conditions such as diabetes and hypertension.
Stage 2: Mild Decrease in Kidney Function (GFR 60–89)
– Mild reductions in kidney efficiency.
– Symptoms may still not be evident.
– Kidney damage continues quietly.
Key Focus:
Regular monitoring and lifestyle changes to avert further decline.
Stage 3: Moderate Kidney Damage (GFR 30–59)
– Waste products begin to accumulate in the bloodstream.
– Symptoms may start to manifest:
– Fatigue
– Swelling (especially in ankles and hands)
– Changes in urination
Key Focus:
Medical treatment becomes increasingly essential; adjustments to diet and medications are often necessary.
Stage 4: Severe Kidney Damage (GFR 15–29)
– Considerable loss of kidney function.
– Symptoms become more apparent and severe.
– Greater risk of complications such as anemia and bone disease.
Key Focus:
Prepare for advanced treatment options such as dialysis or kidney transplant.
Stage 5: Kidney Failure (End-Stage Renal Disease) (GFR < 15)
– The kidneys can no longer function adequately.
– Dangerous levels of waste and fluids build up in the body.
– This is a life-threatening condition.
Treatment Options:
– Dialysis (artificial filtering of blood).
– Kidney transplant.
Why Knowing Your CKD Stage Matters
Every stage of CKD requires a unique level of care and intervention. Early phases can often be managed with lifestyle modifications and appropriate medical attention, while later stages necessitate more intensive treatment.
Regular testing and early diagnosis can significantly slow CKD progression and enhance quality of life.
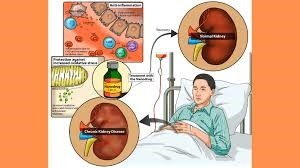
4. Causes of Chronic Kidney Disease
Chronic Kidney Disease does not occur abruptly; rather, it typically results from underlying health conditions that progressively harm the kidneys. Identifying these causes is essential for prevention, prompt intervention, and effective management.
1. Diabetes (Leading Contributor)
Diabetes is the most prevalent cause of chronic kidney disease globally. Elevated blood sugar levels can damage the tiny blood vessels (glomeruli) in the kidneys, impairing their filtering ability.
Effects on the kidneys:
– Thickens the filtering membranes in the kidneys.
– Leads to protein loss in urine (proteinuria).
– Gradually diminishes kidney function.
2. High Blood Pressure
Hypertension stands as another major contributor to CKD. Consistently elevated blood pressure exerts stress on the blood vessels in the kidneys.
Effects include:
– Narrowing or weakening of blood vessels.
– Decreased blood flow to the kidneys.
– Progressive loss of kidney function.
READ ALSO: Early Symptoms of Diabetes In Women: 15 Warning Signs You Shouldn’t Ignore
3. Glomerulonephritis
This encompasses a group of diseases that cause inflammation of the kidney’s filtering units (glomeruli). It can be acute or chronic and may arise from infections, autoimmune disorders, or unidentified causes.
4. Polycystic Kidney Disease (PKD)
A genetic disorder where fluid-filled cysts form in the kidneys, causing enlargement and progressive dysfunction.
5. Recurrent Kidney Infections
Frequent urinary tract infections (UTIs) that reach the kidneys (pyelonephritis) can lead to lasting damage if not treated adequately.
6. Prolonged Use of Certain Medications
Long-lasting use or misuse of certain drugs can harm the kidneys, including:
– Nonsteroidal anti-inflammatory drugs (NSAIDs)
– Specific antibiotics
– Herbal supplements taken without medical oversight.
7. Obstruction of the Urinary Tract
Conditions obstructing urine flow can damage the kidneys, such as:
– Kidney stones
– Enlarged prostate
– Tumors.
8. Autoimmune Diseases
Conditions like lupus can result in the immune system attacking kidney tissues, causing inflammation and long-term damage.
Key Takeaway
Most causes of CKD are preventable or manageable with early diagnosis and appropriate care. Controlling conditions such as diabetes and hypertension is vital for safeguarding kidney health and slowing disease progression.
5. Risk Factors for Chronic Kidney Disease
Chronic Kidney Disease can impact anyone, but certain factors significantly elevate the risk of developing the condition. Understanding these risk factors allows for proactive measures to protect kidney health.
1. Diabetes
Diabetes is the primary risk factor for CKD. Poorly controlled blood sugar levels over time can inflict damage on the filtering system of the kidneys.
2. High Blood Pressure
Hypertension increases stress on the kidney blood vessels, diminishing their ability to filter out waste.
3. Age (60 Years and Older)
As individuals age, kidney function naturally declines. Older adults are more susceptible to kidney damage, especially in conjunction with other health issues.
4. Family History of Kidney Disease
A familial history of kidney disease elevates your risk due to genetic and shared lifestyle factors.
5. Obesity
Excess body weight raises the likelihood of developing conditions such as diabetes and high blood pressure, which in turn can result in CKD.
6. Smoking
Smoking diminishes blood flow to the kidneys, potentially exacerbating any existing kidney injury. It also heightens the risk of cardiovascular diseases.
7. Cardiovascular Disease
Conditions affecting the heart and blood vessels can compromise kidney function because these two systems are intricately interconnected.
8. Poor Diet
Consuming a diet rich in salt, processed foods, and unhealthy fats can put extra strain on the kidneys and lead to elevated blood pressure.
9. Long-Term Use of Harmful Substances
– Prolonged use of pain relievers (particularly NSAIDs)
– Excessive alcohol intake
– Use of unregulated herbal supplements
10. Inadequate Water Intake (Chronic Dehydration)
Insufficient hydration over time can stress the kidneys and diminish their effectiveness.
Key Takeaway
Possessing one or several risk factors does not guarantee you will develop chronic kidney disease (CKD), but it significantly heightens your risk. The encouraging news is that many of these factors can be changed, enabling you to mitigate your risk through lifestyle adjustments, routine health screenings, and appropriate medical care.
6. Symptoms of Chronic Kidney Disease
Chronic Kidney Disease is often referred to as a silent killer, as symptoms tend to manifest only after substantial kidney damage has occurred. During the early stages, many individuals remain asymptomatic, highlighting the importance of regular health checkups—especially for those with risk factors. As kidney function diminishes, waste materials and extra fluids start to accumulate, resulting in noticeable symptoms.
Common Symptoms of CKD
1. Fatigue and Weakness
When kidneys do not operate efficiently, toxins build up in the bloodstream, causing:
– Persistent fatigue
– Low energy
– Trouble concentrating
2. Swelling (Edema)
Inadequate kidney function may lead to fluid retention, resulting in swelling in:
– Legs
– Ankles
– Feet
– Face
3. Urination Changes
Given the kidneys’ role in urine production, CKD can alter urination habits:
– Increased urination (especially nocturnal)
– Decreased urine volume
– Foamy or bubbly urine (indicating protein loss)
– Dark or bloody urine
4. Shortness of Breath
Fluid accumulation in the lungs or anemia from kidney issues can result in breathing difficulties.
5. Nausea and Vomiting
The build-up of waste products can lead to gastrointestinal discomfort, including:
– Nausea
– Vomiting
– Decreased appetite
6. Persistent Itching
Waste accumulation in the blood can cause intense itching (uremic pruritus), particularly in advanced CKD stages.
7. Muscle Cramps
Electrolyte imbalances involving calcium and potassium can result in frequent muscle cramps.
8. Poor Sleep Quality
Individuals with CKD may contend with:
– Insomnia
– Restless legs syndrome
– Disrupted sleep patterns
**Why Symptoms Are Often Overlooked**
Many CKD symptoms are nonspecific and can be confused with other common issues like stress, dehydration, or fatigue, leading to late-stage dagnoses.
When Symptoms Become Severe
In more advanced stages, symptoms may exacerbate to include:
– Significant swelling
– Extreme fatigue
– Mental confusion
– Chest pain (due to fluid around the heart)
Key Takeaway
Do not disregard persistent or unusual symptoms, particularly if you have conditions like diabetes or high blood pressure. Timely detection may slow or even halt the progression of kidney damage.
7. Complications of Chronic Kidney Disease
Chronic Kidney Disease can lead to serious health complications, especially if not diagnosed early or effectively managed. As kidney function deteriorates, the body struggles to maintain fluid, electrolyte, and hormonal balance, impacting virtually every organ system.
1. Anemia
The kidneys produce erythropoietin, a hormone critical for red blood cell production. Declining kidney function can result in:
– Reduced red blood cell creation
– Decreased oxygen delivery to tissues
– Symptoms like fatigue, weakness, and dizziness
2. Heart Disease (Cardiovascular Issues)
CKD substantially raises the risk of cardiovascular conditions such as:
– Heart attack
– Stroke
– Heart failure
These issues arise because kidney health is closely intertwined with heart function, and risk factors like high blood pressure can aggravate both.
3. Fluid Retention (Edema)
Inability to efficiently expel extra fluid can lead to:
– Swelling in legs, ankles, and feet
– Fluid buildups in the lungs (resulting in breathing challenges)
– Elevated blood pressure
4. Electrolyte Imbalance
Kidneys manage crucial minerals like potassium, sodium, and calcium. CKD can disrupt this equilibrium, resulting in:
– High potassium levels (which may affect heart rhythm)
– Muscle weakness and other complications
– Irregular heartbeats
5. Bone Disorder (Renal Osteodystrophy)
The kidneys regulate calcium and phosphorus levels; when they fail:
– Bones may weaken and become fragile
– Increased susceptibility to fractures
– Joint pain
6. Uremia (Toxin Accumulation)
As toxins accumulate, uremia may develop, characterized by:
– Nausea and vomiting
– Loss of appetite
– Mental disorientation
– Severe itching
7. Compromised Immune System
CKD can weaken the immune response, making individuals more susceptible to infections.
8. Nerve Damage (Neuropathy)
Buildup of toxins and electrolyte disturbances may injure nerves, leading to:
– Tingling or numbness
– Burning sensations
– Muscle weakness
9. Pregnancy Risks
Women with CKD may encounter increased risks during pregnancy, including:
– High blood pressure
– Preterm birth
– Complications for both the mother and child
10. Kidney Failure (End-Stage Renal Disease)
This is the most critical consequence, wherein kidneys fail to function adequately. At this stage:
– Waste and fluid accumulation can become life-threatening
– Treatment options typically involve dialysis or kidney transplantation
Key Takeaway
The complications associated with CKD can be severe, but many can be prevented or effectively managed with timely diagnosis, appropriate treatment, and lifestyle changes. Managing underlying conditions such as diabetes and high blood pressure is vital for reducing these risks.
8. Diagnosing Chronic Kidney Disease
Early diagnosis of Chronic Kidney Disease is essential for slowing its progression and averting severe complications. Since CKD often develops without clear symptoms, medical evaluations are crucial for detecting the condition even before symptoms arise.
Doctors typically utilize a mix of blood tests, urine analyses, and imaging assessments to evaluate kidney function and detect any damage.
1. Blood Tests
Blood tests are among the pivotal tools for CKD diagnosis.
– Serum Creatinine Test: Assesses the level of creatinine (a waste product) in the blood; elevated levels may indicate poor kidney functioning.
– Glomerular Filtration Rate (GFR): Calculated using creatinine levels, age, sex, and additional factors to indicate kidney filtration efficiency.
Why it matters: A low GFR serves as a significant marker of kidney disease, helping determine CKD stages.
2. Urine Tests
Urine analysis identifies abnormalities suggesting kidney damage.
– Protein in Urine (Proteinuria):** One of the earliest indicators of CKD
– Albumin-to-Creatinine Ratio (ACR):** Evaluates the extent of protein leakage
– Urinalysis: Detects blood, infections, or other irregularities
3. Imaging Studies
Imaging tests offer a visual representation of the kidneys and assist in spotting structural concerns.
– Ultrasound: Reveals kidney size, shape, and any potential obstructions
– CT Scan or MRI: Provides more in-depth imaging as required
4. Kidney Biopsy
In certain situations, a small sample of kidney tissue is extracted and analyzed under a microscope.
Purpose:
– To pinpoint the exact cause of kidney damage
– To gauge disease severity
– To inform treatment choices
5. Blood Pressure Monitoring
Regular monitoring is crucial during diagnosis and treatment since high blood pressure both contributes to and exacerbates CKD.
Who Should Be Tested?
Consider regular kidney function assessments if you:
– Have diabetes
– Have high blood pressure
– Have a family history of kidney disease
– Are over 60 years of age
– Experience symptoms like fatigue, swelling, or changes in urination
Key Insight
Timely identification of Chronic Kidney Disease (CKD) is crucial for effective management. Regular screening—particularly for those at higher risk—enables prompt treatment, which can slow the progression of the disease and enhance quality of life.
9. Managing Chronic Kidney Disease
The management of CKD is centered on decelerating disease advancement, alleviating symptoms, and warding off complications. While curing CKD is not always feasible, proactive and sustained treatment can empower many individuals to live extended, healthy lives. Treatment strategies are typically tailored to the disease’s stage, its underlying causes, and the overall health of the individual.
1. Addressing Root Causes
The primary focus should be on controlling the health issues that caused kidney damage.
– Diabetes Management: Implement a suitable diet, use medications, and continually monitor blood sugar levels.
– High Blood Pressure Control: Adopt lifestyle modifications and utilize prescribed medications.
Objective: Prevent additional kidney damage.
2. Medications
Healthcare providers may recommend medications to ease symptoms and minimize complications:
– Blood pressure medications such as ACE inhibitors or ARBs for kidney protection.
– Diuretics to eliminate fluid retention and swelling.
– Erythropoietin-stimulating agents to combat anemia.
– Phosphate binders to safeguard bones.
– Statins for cholesterol reduction.
3. Lifestyle Adjustments
Lifestyle changes are vital for CKD management.
– Embrace a kidney-friendly diet (low sodium, moderated protein).
– Keep a healthy body weight.
– Engage in regular physical activity.
– Cease smoking.
– Limit alcohol intake.
4. Dietary Considerations
Diet significantly influences the slowing of CKD progression.
Recommendations:
– Incorporate fresh fruits and vegetables (considering potassium content).
– Opt for whole foods over processed items.
– Ensure proper hydration as per medical advice.
Restrict or Eliminate:
– High-sodium items.
– Excess protein (notably in later stages).
– Foods containing high potassium and phosphorus (if instructed).
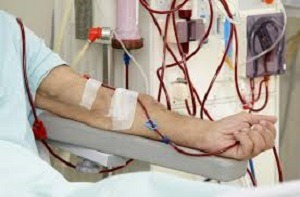
5. Dialysis (For Advanced Stages)
When kidney function declines to critical levels (Stage 5), dialysis may become necessary.
Dialysis Types:
– Hemodialysis: Machine-assisted blood filtration.
– Peritoneal Dialysis: Utilizes the abdominal lining for filtration.
Purpose: To remove toxins and excess fluids when the kidneys can no longer cope.
6. Kidney Transplant
A kidney transplant replaces a failing kidney with a donor’s healthy organ.
**Benefits:**
– Enhanced quality of life.
– Fewer dietary restrictions compared to dialysis.
Considerations:
– Requires lifelong medication for organ rejection prevention.
7. Holistic and Supportive Approaches
While medical interventions are critical, complementary natural strategies can bolster health:
– Consume foods rich in antioxidants.
– Manage stress effectively.
– Steer clear of unsafe herbal remedies without professional guidance.
– Maintain physical activity.
Key Insight
CKD management is most effective when combining medical intervention, lifestyle modifications, and early detection. Early diagnosis and treatment significantly enhance the likelihood of slowing disease progression and circumventing severe complications.
10. Natural and Lifestyle Strategies
Effectively managing Chronic Kidney Disease extends beyond medication—daily habits greatly influence the pace of its decline and overall health enhancement. While these natural approaches do not substitute for medical therapy, they can be instrumental in sustaining kidney health when properly implemented.
1. Adhere to a Kidney-Friendly Diet
Diet remains one of the most potent tools in CKD management.
Focus on:
– Fresh fruits and vegetables (per your physician’s guidance).
– Whole, unprocessed foods.
– Low-sodium dishes.
Importance: Lowering salt helps manage high blood pressure and avoids fluid retention.
2. Ensure Proper Hydration
Adequate water intake assists the kidneys in detoxification.
– Avoid both dehydration and excessive hydration.
– Adhere to your physician’s guidelines, especially during advanced CKD stages.
3. Manage Blood Sugar Levels
For those with Diabetes, keeping blood sugar within ideal parameters is vital for preventing further renal damage.
4. Achieve a Healthy Weight
Being overweight enhances the risk of kidney strain and associated complications.
– Target slow, sustainable weight reduction if needed.
– Merge dietary efforts with consistent physical activity.
5. Regular Physical Activity
Exercise boosts overall wellness and enhances kidney performance.
Recommended Activities:
– Walking.
– Light jogging.
– Cycling.
– Yoga.
Aim for a minimum of 30 minutes of moderate exercise most days.
6. Limit Sodium Intake
Excessive salt can aggravate fluid retention and elevate blood pressure.
– Avoid processed and packaged food.
– Curb intake of fast food and salty snacks.
– Use natural herbs and spices in place of salt.
7. Cautious Use of Painkillers
Overusing certain medications (like NSAIDs) can lead to chronic kidney issues.
– Use medications strictly as directed.
– Consult with your physician prior to any long-term usage.
8. Be Cautious with Herbal Remedies
Not every natural remedy is suitable for kidney health.
– Avoid unverified herbal supplements.
– Always discuss herbal treatments with your healthcare provider beforehand.
9. Quit Smoking
Smoking diminishes blood circulation to the kidneys and speeds up damage.
– Quitting enhances both general and renal health.
10. Effectively Manage Stress
Chronic stress can adversely affect blood pressure and overall well-being.
Beneficial Techniques:
– Meditation.
– Deep breathing.
– Relaxation strategies.
11. Routine Medical Checkups
Regular health assessments assist in early detection and treatment plan modifications.
Key Insight
Implementing simple lifestyle changes can greatly influence CKD management. By merging healthy routines with appropriate medical care, individuals can decelerate disease progress, diminish complications, and enhance their quality of life.
11. Dietary Guidelines for CKD
Diet is fundamental in managing Chronic Kidney Disease. Thoughtful food choices can alleviate the workload on kidneys, control symptoms, and impede disease advancement. Dietary requirements may vary based on CKD stages, so individualized medical recommendations are crucial.
Foods to Include (Kidney-Friendly Selections)
1. Low-Potassium Fruits
– Apples.
– Berries (e.g., strawberries, blueberries).
– Grapes.
– Pineapple.
Reasoning: Prevents potassium overaccumulation, critical in advanced CKD.
2. Low-Potassium Vegetables
– Cabbage.
– Carrots.
– Cucumbers.
– Lettuce.
3. Moderate Healthy Proteins
– Fish.
– Skinless chicken.
– Eggs.
Note: Protein intake should be moderated to prevent kidney strain.
4. Controlled Portions of Whole Grains
– White rice (typically preferable in advanced CKD due to lower phosphorus).
– Oats.
– Pasta.
5. Healthy Fats
– Olive oil.
– Avocados (served in moderation based on potassium levels).
6. Sufficient Fluids
– Water (as per medical advice).
– Low-sugar beverages.
Foods to Limit or Avoid
1. High-Sodium Items
– Processed foods (instant noodles, canned soups).
– Fast foods.
– Salty snacks.
Reasoning: Excess salt exacerbates high blood pressure and fluid retention.
2. High-Potassium Foods (Particularly in Advanced CKD)
– Bananas.
– Oranges.
– Potatoes.
– Tomatoes.
3. High-Phosphorus Foods
– Dairy products (milk, cheese).
– Processed meats.
– Sugary sodas (cola).
4. Excessive Protein
– Large servings of red meat.
– Protein supplements without medical advice.
5. Sugary Treats and Beverages
– Sodas.
– Pastries.
– Candies.
These can exacerbate Diabetes, which is a major contributor to CKD.
6. Alcohol
– Can increase blood pressure.
– Imposes additional strain on the kidneys.
Essential Dietary Tips
– Always inspect food labels for sodium and phosphorus content.
– Prepare meals at home for better ingredient control.
– Opt for smaller, balanced meals.
– Consult a dietitian for a personalized nutrition plan.
Key Insight
There isn’t a universal diet for CKD, but making informed food choices can significantly enhance kidney health. A well-rounded, kidney-friendly eating plan aids in alleviating symptoms, thwarting complications, and promoting overall wellness.
2. Prevention Strategies
While Chronic Kidney Disease may not always be entirely preventable, many instances can be postponed or averted through healthy lifestyle practices and effective management of pre-existing conditions. Prevention is crucial for those at heightened risk.
1. Manage Blood Sugar Levels
Effectively controlling Diabetes is one of the best defenses for kidney preservation.
– Regularly check blood sugar levels.
– Adhere to a healthy diet.
– Use prescribed medications diligently.
2. Maintain Optimal Blood Pressure
Keeping high blood pressure in check reduces stress on the kidneys.
– Decrease salt intake.
– Engage in regular physical activity.
– Consistently monitor blood pressure.
3. Stay Hydrated
Proper hydration supports the kidneys in efficiently removing toxins.
– Strive for steady daily water consumption.
– Adjust fluid intake depending on health status.
4. Follow a Nutrient-Rich Diet
A well-rounded diet is essential for optimal kidney health.
– Emphasize fresh, unprocessed foods
– Reduce intake of processed and high-salt items
– Pay attention to portion control
5. Stay Physically Active
Regular exercise promotes a healthy weight and boosts circulation.
– Strive for at least 30 minutes of moderate activity most days
– Engage in activities like walking, cycling, or swimming for best results
6. Steer Clear of Smoking
Smoking harms blood vessels and diminishes kidney blood flow, raising the risk of kidney issues.
7. Use Medications Wisely
Excessive use of certain medications can harm your kidneys.
– Limit the intake of pain relievers (NSAIDs)
– Always adhere to medical guidance when using any medication
8. Limit Alcohol Consumption
Drinking too much alcohol can elevate blood pressure and gradually damage the kidneys.
9. Schedule Regular Health Checkups
Routine examinations help catch kidney issues early on—before any symptoms manifest.
– Monitor blood pressure
– Evaluate blood sugar levels
– Conduct kidney function tests if at risk
10. Keep a Healthy Weight
Carrying excess weight raises the chances of developing conditions that may result in CKD.
– Pair a nutritious diet with frequent exercise
– Seek gradual and consistent weight loss if necessary
Key Takeaway
Preventing CKD involves taking charge of your health early. Simple habits like eating well, exercising, and keeping track of your health can significantly safeguard your kidneys and overall health.
13. When to Consult a Doctor
Early intervention is crucial in managing Chronic Kidney Disease. Since symptoms often surface late, seek medical attention at the first sign of unusual changes in your body, especially if you’re at risk.
Consult a physician right away if you notice:
– Persistent swelling in the legs, ankles, feet, or face
– Alterations in urination (frequency, color, or foamy appearance)
– Ongoing fatigue or weakness
– Shortness of breath
– Nausea or a decrease in appetite
– Difficulty concentrating or feelings of confusion
High-Risk Individuals Should Seek Regular Testing
Don’t wait for symptoms to arise if you:
– Have Diabetes
– Suffer from High Blood Pressure
– Have a family history of kidney disease
– Are over 60 years old
Key Takeaway
Don’t overlook early warning signs. Regular testing and prompt medical attention can help identify CKD in its early stages and avert severe complications.
14. Common Questions (FAQs)
1. Is there a cure for chronic kidney disease?
No, while Chronic Kidney Disease isn’t always curable, it can be effectively managed. Early intervention can decelerate its advancement.
2. How quickly does CKD advance?
Progression is unique to each individual. With proper management of conditions like Diabetes and High Blood Pressure, the disease can develop slowly.
3. Is CKD life-threatening?
Yes, untreated CKD may result in kidney failure and serious issues like heart disease. However, early detection greatly enhances outcomes.
4. Can you lead a normal life with CKD?
Absolutely, many individuals live fulfilling lives with CKD by adhering to treatment plans, maintaining a healthy lifestyle, and keeping regular checkups.
5. What diet is best for CKD patients?
A kidney-friendly diet features low sodium, limited protein, and balanced nutrients. The specific diet varies based on the disease stage.
6. Are herbal treatments safe for kidney disease?
Not all herbal remedies are safe; some may worsen kidney damage. Always seek professional advice before trying any herbal products.
READ ALSO: 7 Best Treatments For Stroke: Effective Options For Recovery And Prevention
7. How can I identify kidney disease early?
Regular blood and urine testing is the most reliable method for early CKD detection, especially if you’re at risk.
15. Conclusion
Chronic Kidney Disease is a serious condition, yet it can be managed effectively. Understanding its causes, recognizing early warning signs, and taking proactive measures can be life-saving.
From managing Diabetes and High Blood Pressure to embracing a healthy lifestyle and following medical guidance, every action contributes to preserving your kidney health.
The essential message is clear: early detection and consistent care can extend life, prevent complications, and enhance your quality of life. Don’t wait for symptoms—prioritize your health now.