What Causes Testicular Pain? 12 Key Reasons Men Must Not Overlook
Introduction
Testicular pain encompasses any discomfort or soreness in one or both testicles, varying from mild, dull discomfort to sudden, intense pain. It is generally categorized as acute testicular pain, which appears suddenly and may indicate a medical emergency, or chronic testicular pain, lasting weeks or months and possibly linked to underlying health issues that need medical assessment. Regardless of intensity, testicular pain should never be taken lightly.
Disregarding testicular pain can be hazardous, as it might be an indicator of serious health problems like infections, reduced blood supply to the testicles, or even testicular cancer. Some conditions, such as testicular torsion, can result in permanent damage or testicular loss if not treated immediately. Timely medical attention significantly enhances the likelihood of effective treatment, protecting long-term fertility and sexual health.
This article aims to inform men of all ages—from teenagers to seniors—about testicular pain, as it can arise at any life stage. Recognizing whether the pain is sudden, ongoing, mild, or severe enables you to make educated health decisions.
Fortunately, many causes of testicular pain are manageable, particularly when diagnosed early. Seeking medical help quickly can provide reassurance, avert complications, and address serious conditions before they escalate.
What Is Testicular Pain? (Quick Overview)
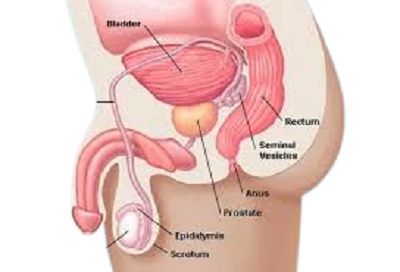
Testicular pain refers to any discomfort, ache, or acute pain experienced in one or both testicles, the oval-shaped glands located within the scrotum. The pain may arise abruptly or gradually and can range in intensity from mild annoyance to extreme, debilitating pain affecting daily tasks.
Differentiating testicular pain from groin or scrotal pain is crucial. Testicular pain originates directly from the testicles, often resulting from conditions impacting blood supply, infections, inflammation, or injuries. In contrast, groin or scrotal pain might stem from surrounding tissues like muscles, nerves, the lower abdomen, or the inguinal canal, causing discomfort around—but not directly in—the testicles.
Testicular pain can be unilateral (affecting one testicle) or bilateral (affecting both). Pain in one testicle is frequently associated with conditions such as testicular torsion, injuries, or infections, while bilateral pain may relate to systemic infections, inflammation, or referred pain from other bodily areas.
The pain type can also provide vital clues regarding its cause. Some men report a mild or dull ache that intensifies with activity or prolonged standing. Others may experience sharp or stabbing pain, indicating a potential emergency. Occasionally, the pain can radiate to the lower abdomen, groin, back, or inner thigh, suggesting nerve involvement or referral from another organ. Recognizing these patterns assists healthcare professionals in determining the cause and the necessary treatment.
12 Common Causes of Testicular Pain
Various conditions can lead to testicular pain—some benign and temporary, while others serious and requiring immediate medical attention. Here are 12 common causes of testicular pain every man should know.
1. Testicular Torsion (Emergency)
This condition happens when the spermatic cord twists, interrupting blood flow to the testicle. It results in sudden, severe pain, swelling, nausea, and sometimes vomiting. Testicular torsion is a medical emergency that requires urgent surgery to avoid permanent damage or loss of the testicle.
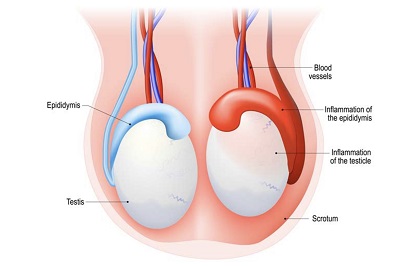
2. Epididymitis
Epididymitis involves inflammation of the epididymis, the tube that carries and stores sperm, often caused by bacterial infections, including STIs. Symptoms include gradual pain, swelling, warmth, and sometimes fever or painful urination.
3. Orchitis
Orchitis refers to the inflammation of one or both testicles, usually due to viral or bacterial infections, with mumps being a notable viral cause. Symptoms may include testicular pain, swelling, tenderness, and flu-like symptoms.
4. Varicocele
A varicocele is an enlargement of veins in the scrotum resembling varicose veins. It typically causes a dull ache or heaviness, especially after standing for extended periods or during physical exertion.
5. Inguinal Hernia
An inguinal hernia occurs when part of the intestine protrudes through a weak point in the abdominal wall into the groin, potentially causing testicular discomfort, pressure, or pain that worsens with coughing or lifting.
6. Kidney Stones
Kidney stones can produce referred pain radiating from the lower back or abdomen into the groin and testicles. This pain is often intense and may be accompanied by nausea, vomiting, or blood in the urine.
7. Testicular Injury or Trauma
Injury to the testicles from sports, accidents, or falls can lead to immediate pain and swelling. While minor injuries may resolve naturally, persistent or worsening pain following trauma should be assessed by a healthcare provider.
8. Sexually Transmitted Infections (STIs)
STIs like chlamydia and gonorrhea can cause infections in the epididymis or testicles. Symptoms may include testicular pain, swelling, discharge, and burning during urination.
9. Prostatitis
Prostatitis is inflammation of the prostate gland, which can cause pain radiating to the testicles, pelvis, or lower back. Other symptoms may include painful urination, difficulty urinating, or discomfort during ejaculation.
10. Hydrocele
A hydrocele refers to fluid accumulation around the testicle, generally leading to swelling and a sensation of heaviness, though discomfort can arise as the fluid buildup increases.
11. Spermatocele
A spermatocele is a benign cyst filled with fluid that develops in the epididymis. It typically causes little to no pain but may produce a dull ache, pressure, or a noticeable lump in the scrotum.
12. Testicular Cancer
While testicular cancer is often asymptomatic in its early stages, it can sometimes lead to discomfort, heaviness, or a dull ache in the testicles. Any persistent lump, size change, or unexplained pain should be promptly evaluated.

What Causes Testicular Pain Without Swelling?
Testicular pain doesn’t always accompany visible swelling. Many men experience discomfort or pain even when the testicles appear normal. This type of pain can be perplexing and is often associated with nerve-related issues, referred pain, or initial-stage medical conditions.
Here are common reasons for testicular pain without swelling:
1. Nerve-Related Pain (Neuropathic Pain)
Nerve irritation or compression in the lower back, pelvis, or groin can lead to pain in the testicles. Conditions like lumbar disc problems, sciatica, or nerve entrapment may trigger sharp, burning, or tingling sensations without any visible changes to the scrotum.
2. Referred Pain From Nearby Organs
Testicular pain can stem from adjacent structures and be “referred” to the testicles. Typical sources include:
– Kidney stones
– Urinary tract infections
– Appendicitis (initial stages)
– Strains in lower abdominal or pelvic muscles
In these situations, the testicles themselves remain unaffected, leading to an absence of swelling.
3. Early-Stage Infections
Conditions like epididymitis or orchitis may first induce pain before swelling or redness appear. Initial symptoms can include mild to moderate discomfort, aching, or tenderness that exacerbates over time without treatment.
4. Chronic Testicular Pain (Orchialgia)
Chronic orchialgia refers to testicular discomfort that lasts three months or more without a clear cause. This condition may stem from prior injuries, surgeries (like vasectomies), nerve sensitivity, or ongoing inflammation, even when clinical examinations and imaging appear normal.
5. Prostatitis
Inflammation of the prostate gland can lead to pain that radiates to the testicles, without causing noticeable swelling. Other symptoms may include pelvic discomfort, painful urination, and pain during ejaculation.
6. Muscle Strain or Pelvic Floor Dysfunction
Straining the pelvic floor or groin muscles from overexertion, heavy lifting, prolonged sitting, or vigorous exercise can result in a dull or pulling sensation in the testicles, typically without accompanying swelling.
7. Psychological Stress and Anxiety
Anxiety and stress can lead to increased muscle tension and an amplified sense of pain, occasionally resulting in discomfort in the testicles despite the absence of a physical problem. This pain is often alleviated once stress is relieved.
When to Be Concerned
Testicular pain should not be overlooked if it:
– Lingers for more than a few days
– Becomes acute or intense suddenly
– Accompanies fever, nausea, or urinary issues
– Disrupts daily functioning
In these scenarios, a medical evaluation is essential to rule out severe conditions and to ensure suitable treatment.
What Causes Sudden Testicular Pain?
Experiencing sudden testicular pain can be alarming—and rightly so. Abrupt pain, especially if it’s intense, may indicate a medical emergency necessitating immediate care. While some causes might be benign, others could compromise testicular health without timely intervention.
Here are the most common reasons for sudden testicular pain:
1. Testicular Torsion (Emergency Condition)
Testicular torsion is the primary cause of abrupt, severe testicular pain. This condition arises when the spermatic cord twists, cutting off the blood supply to the testicle. Symptoms may include:
– Sudden intense pain
– Swelling and redness in the scrotum
– Nausea and vomiting
– One testicle positioned higher than the other
This is a medical emergency requiring treatment within 4–6 hours to preserve the testicle.
2. Testicular Injury or Trauma
A direct impact to the testicles from sports, accidents, or falls can cause immediate pain. While mild injuries might improve with rest, persistent or worsening discomfort post-trauma could suggest internal bleeding or damage and should be evaluated promptly.
3. Acute Epididymitis
Although epididymitis typically develops gradually, it can sometimes present with sudden pain, particularly when triggered by a bacterial infection. Symptoms may include fever, painful urination, or tenderness in the scrotum.
4. Incarcerated Inguinal Hernia
When a hernia becomes trapped (incarcerated), it can abruptly inhibit blood flow to tissues in the groin, resulting in sharp pain in the testicles or groin, along with swelling, nausea, and vomiting. This situation demands urgent medical attention.
5. Kidney Stones (Referred Pain)
Kidney stones can lead to sudden, intense pain that radiates from the lower back to the groin and testicles, often described in waves and may be accompanied by nausea, vomiting, or blood in the urine.
6. Testicular Appendage Torsion
This condition occurs when a small remnant of tissue near the testicle twists, causing sudden pain akin to testicular torsion but is usually less severe. A small blue dot might appear on the scrotum. Medical evaluation is necessary to rule out true torsion.
7. Sudden Nerve Compression
Abrupt nerve irritation due to lower back problems, awkward movements, or extended sitting can trigger sharp or shooting pain in the testicles without swelling. While generally not dangerous, persistent pain should be assessed.

When Sudden Testicular Pain Is an Emergency
Seek emergency medical care if sudden testicular pain:
– Is intense or escalating
– Lasts longer than 30–60 minutes
– Accompanies nausea, vomiting, or fever
– Follows an injury
– Includes scrotal swelling or redness
Prompt attention can help avoid complications and safeguard long-term fertility and sexual health.
When Should You See a Doctor for Testicular Pain?
While mild testicular discomfort can sometimes resolve independently, persistent, severe pain, especially with other symptoms, should be addressed seriously. Recognizing the right time to seek medical attention can prevent serious issues and protect reproductive health.
You should visit a doctor urgently or seek emergency care for the following symptoms:
Seek Urgent Medical Attention If:
– Sudden, intense testicular pain without an evident cause
– Pain lasting over 30–60 minutes without relief
– Scrotal swelling, redness, or warmth
– Nausea or vomiting paired with testicular pain
– Fever or chills, possibly indicating infection
– One testicle positioned unusually or higher than the other
– Pain following trauma or injury to the groin
– Difficulty urinating, painful urination, or blood in urine
– Penile discharge or signs of a sexually transmitted infection
These signs may suggest emergencies such as testicular torsion, severe infections, or incarcerated hernias, all needing immediate treatment.
See a Doctor Soon (Within a Few Days) If:
– Testicular pain persists beyond a few days
– Pain is mild but recurrent
– A lump, heaviness, or change in size or shape of the testicle is noticed
– Pain is accompanied by pelvic, groin, or lower back discomfort
– You have a personal history of urinary or prostate issues
Routine Medical Evaluation Is Important If:
– Chronic testicular pain lasts longer than 3 months
– Pain impacts daily life, work, or sexual activity
– History of previous scrotal surgeries or vasectomies
– Uncertainty about the cause and need for reassurance
Key Takeaway
It’s essential to approach testicular pain with caution. Early medical assessment can rule out severe conditions, alleviate anxiety, and facilitate timely intervention. Delaying care may lead to complications, such as infertility or enduring testicular harm.
How Is Testicular Pain Diagnosed?
To identify the cause of testicular pain, a physician will start with a comprehensive medical history and physical examination. Patients may need to describe when the pain started, its severity, its onset (sudden or gradual), and any accompanying symptoms like fever, urinary issues, or recent trauma.
Common diagnostic procedures include:
– Physical examination: Assessing the testicles, scrotum, groin, and abdomen for signs of swelling, tenderness, lumps, or abnormal positioning.
– Scrotal ultrasound: A non-invasive imaging technique that tests blood flow and helps diagnose torsion, infection, cysts, or tumors.
– Urine tests: Used to detect urinary tract infections or sexually transmitted infections.
– Blood tests: May be necessary if infection or inflammation is suspected.
– STI screening: Particularly vital for sexually active men presenting with symptoms of infection.
These evaluations assist in ruling out emergencies and determining the most appropriate course of treatment.
Treatment Options for Testicular Pain
Treatment is contingent on the underlying cause. Some conditions necessitate urgent action, while others respond to medication or conservative therapy.
Common treatment methods include:
– Emergency surgery: Required for testicular torsion to restore blood flow and preserve the testicle.
– Antibiotics: Prescribed for bacterial infections such as epididymitis, orchitis, or STIs.
– Pain relief and anti-inflammatory medications: Aimed at alleviating discomfort and swelling.
– Supportive care: Employing scrotal support, rest, ice packs, and elevation for mild cases or injuries.
– Surgical repair: May be required for hernias, significant varicoceles, or persistent hydroceles.
– Chronic pain management: Involving physical therapy, nerve treatments, or specialist referrals for long-lasting orchialgia.
Self-treatment without professional guidance is not advisable, especially for severe or persistent pain.
Common Questions (CQs) Regarding Testicular Pain
1. Is testicular pain a serious issue?
Not necessarily. Mild cases can be temporary, resulting from minor injuries, muscle strain, or transient inflammation. However, if you experience sudden or intense pain, swelling, or any other alarming symptoms, a serious condition may be present, warranting immediate medical evaluation.
2. Can testicular pain resolve without treatment?
Minor discomfort may clear up on its own, especially if it stems from brief strain, small injuries, or mild infections. However, ongoing, recurrent, or severe pain should always be taken seriously.
READ ALSO: 7 Ear Infection Home Treatments: Safe Remedies And Medical Care
3. Does testicular pain affect fertility?
Yes. Issues like testicular torsion, infections, varicocele, or untreated chronic inflammation can diminish sperm production or quality, thereby impacting fertility. Prompt diagnosis and treatment are crucial.
4. When should I seek medical attention for testicular pain?
If you experience sudden or severe pain, along with swelling, nausea, or fever, you should seek medical help immediately. For mild pain lasting more than a few days or recurring pain, it’s essential to have a medical assessment soon.
5. Can stress lead to testicular pain?
While stress or anxiety can induce discomfort or a dull ache due to muscle tension or referred nerve pain, they do not cause serious testicular issues. Any persistent or intense pain should be evaluated by a healthcare professional.
6. How is testicular pain different from scrotal pain?
Testicular pain originates from the testicles, whereas scrotal pain relates to surrounding tissues, skin, or fluid-filled sacs like a hydrocele. Sometimes pain can be referred from adjacent areas.
7. Can infections result in sudden testicular pain?
Yes. Conditions like epididymitis or orchitis may initially manifest gradually but can escalate quickly. Severe infections might bring about swelling, fever, and acute pain.
8. What distinguishes testicular torsion from other causes of pain?
Testicular torsion happens when the spermatic cord twists, halting blood flow. It induces sudden, intense pain, swelling, nausea, and sometimes vomiting. Immediate surgical intervention is necessary to rescue the testicle.
9. Are all lumps indicative of cancer?
No. Lumps may arise from benign issues like cysts, hydrocele, or varicocele. Nevertheless, any new lump warrants evaluation by a healthcare provider to exclude testicular cancer.
10. What should I do if I’m uncertain about my symptoms?
If you’re unsure about the cause of your testicular pain, it’s best to seek a medical evaluation without delay. Early diagnosis can prevent complications, safeguard fertility, and ensure appropriate treatment.
Conclusion
Testicular pain is a serious symptom that requires attention—not speculation. While some causes may be benign and fleeting, others—like testicular torsion, infections, or cancer—can lead to severe outcomes if neglected. Recognizing potential causes, identifying red flags, and pursuing prompt medical care are vital in protecting your reproductive well-being. If you experience sudden, intense, or ongoing testicular pain, don’t hesitate—swift diagnosis and intervention can avert complications, maintain fertility, and bring reassurance.