What Causes Peyronie’s Disease in Men? (Complete Guide)
Introduction
Peyronie’s Disease is a condition that affects numerous men but is often misconceived, underreported, or overlooked due to feelings of shame. It emerges when fibrous scar tissue—referred to as plaque—forms inside the penis, resulting in a bend, curve, or distortion of its usual shape during erection. Although a slight natural curve can be normal, Peyronie’s Disease generally involves a marked alteration that may be painful and disrupt sexual performance and self-esteem.
One prevalent question men have is: “What precisely triggers Peyronie’s Disease?” The explanation is not always simple. In many instances, it stems from repeated minor injuries to the penis—often occurring during sexual activity—that do not heal adequately. Over time, this leads to inflammation and the buildup of hardened scar tissue. However, not every case is related to evident trauma. Factors such as aging, genetics, underlying medical issues, and lifestyle choices can also contribute significantly.
Understanding the underlying causes of Peyronie’s Disease is crucial for early identification, prevention, and effective management. When detected early, the progression of this condition can frequently be slowed or treated more efficiently. Unfortunately, many men postpone seeking help until they experience severe symptoms, which may limit their treatment alternatives.
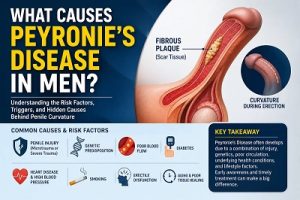
In this guide, you’ll discover the true causes of Peyronie’s Disease in men, the primary risk factors to be aware of, and how everyday behaviors may influence your chances of developing this condition.
What Is Peyronie’s Disease? (Quick Overview)
Peyronie’s Disease is a medical condition characterized by the formation of fibrous scar tissue (known as plaque) within the penis, resulting in an abnormal curvature, particularly during an erection. Unlike the slight natural bend some men possess, this condition typically leads to a marked and sometimes progressive distortion in shape.
The plaque forms beneath the skin of the penis, usually along the shaft, reducing tissue flexibility. Consequently, when the penis becomes erect, the affected area does not stretch adequately, leading to a curve, shortening, or even narrowing at certain points.
Key Characteristics
• A visible bend or curve in the penis (upward, downward, or sideways)
• Hard lumps or thickened areas felt beneath the skin
• Pain during erection (more common in early stages)
• Difficulty achieving or sustaining an erection
• Shortening of the penis in certain instances
How It Affects Men
Peyronie’s Disease can range from mild to severe. In mild cases, the curvature might not disrupt sexual activity. However, in more advanced cases, it can result in painful erections, erectile dysfunction, and challenges with penetration. Beyond the physical symptoms, it can also diminish a man’s confidence, relationships, and overall quality of life.
Is It a Common Condition?
While many men may feel reluctant to discuss it, Peyronie’s Disease is relatively prevalent—particularly among men over 40. Nonetheless, younger men can also experience the condition, especially if there has been trauma or other underlying risk factors.
Comprehending what Peyronie’s Disease is provides the groundwork for identifying its causes, recognizing early symptoms, and obtaining appropriate treatment promptly.
What Causes Peyronie’s Disease in Men?
Understanding the primary causes is vital for prevention and early intervention. While the exact trigger isn’t always apparent, most instances link back to injury and abnormal healing within the penis.
1. Repeated Minor Injury (Microtrauma)
This is the most frequent cause.
• Small, often unnoticed injuries can occur during:
◦ Sexual activity
◦ Physical sports or activities
• Such minor injuries harm blood vessels in the penis
• Instead of healing correctly, the body forms scar tissue (plaque)
Over time, repetitive microtrauma results in the accumulation of plaque, leading to curvature.
2. Sudden or Severe Penile Injury
In some situations, the cause is more evident.
• A sharp bend during intercourse
• Accidental injury (e.g., impact or forceful movement)
• “Penile fracture” (rare but serious)
This type of trauma can prompt:
• Internal bleeding
• Inflammation
• Rapid scar tissue development
3. Abnormal Healing Response
Not all individuals heal identically.
• The body might create excess collagen during healing
• This results in thick, rigid scar tissue rather than flexible tissue
• The plaque does not stretch like normal tissue, causing bending
This clarifies why some men develop the condition even after minor injuries.
4. Genetic Factors
Family history may elevate your risk.
• Some men inherit a predisposition for abnormal scar formation
• It is associated with connective tissue disorders such as Dupuytren’s contracture
• If a close family member has it, your likelihood may be increased
5. Aging and Reduced Tissue Elasticity
Age significantly influences the condition.
• As men age:
◦ Penile tissue becomes less elastic
◦ Healing processes slow down
• This makes injuries more probable and recuperation less efficient
That’s why Peyronie’s Disease is more frequently seen in men over 40.
6. Poor Blood Flow and Underlying Health Issues
Certain health conditions contribute indirectly:
• Diabetes
• High blood pressure
• Cardiovascular diseases
These issues:
• Reduce blood circulation
• Hinder healing
• Heighten scar formation risk
7. Erectile Dysfunction (ED)
A strong correlation exists between ED and Peyronie’s Disease.
• Weak erections reduce penile rigidity
• This raises the chance of bending during intercourse
• Repeated bending may lead to injury and plaque buildup
8. Inflammation and Autoimmune Response
In some cases, the body might react abnormally:
• Chronic inflammation in penile tissue
• Possible autoimmune response (the body attacking its own tissue)
This can incite scar tissue development even without clear injury.
Key Takeaway
In most instances, Peyronie’s Disease arises from a mixture of:
• Injury (minor or major)
• Poor or aberrant healing
• Underlying risk factors (age, health conditions, genetics)
This is why early awareness and preventive strategies are essential.
Risk Factors That Increase the Chances
While injury and healing complications are the main causes, certain factors can considerably enhance your likelihood of developing Peyronie’s Disease. These risk factors don’t directly cause the condition but make the penile tissue more susceptible to damage and poor repair.
1. Age (Especially Over 40)
• Risk escalates as men age
• Penile tissue loses elasticity and becomes more fragile
• Healing processes slow down
This increases the chances of even minor injuries resulting in scar tissue formation.
2. Genetic Predisposition
• Family history influences risk
• Men with relatives who have Peyronie’s Disease are more likely to be affected
• Strongly associated with connective tissue disorders like Dupuytren’s contracture
If your body tends to produce dense scar tissue, your risk increases.
3. Erectile Dysfunction (ED)
• Weak or incomplete erections heighten bending risk during intercourse
• Lack of rigidity makes the penis more vulnerable to injury
• Repeated strain can eventually lead to plaque buildup
ED and Peyronie’s Disease often coincide.
4. Diabetes
• Poor blood sugar management damages blood vessels
• Diminishes blood flow to the penile tissue
• Slows down healing and raises scar formation risk
Men with diabetes are notably more likely to develop this condition.
5. Smoking
• Harms blood vessels and decreases circulation
• Disrupts tissue repair
• Enhances inflammation throughout the body
Smoking is a significant but avoidable risk factor.
6. High Blood Pressure and Heart Disease
• Impacts blood vessel health
• Limits oxygen and nutrient delivery to tissues
• Contributes to slower healing post-injury
These conditions indirectly encourage plaque development.
7. Prostate Surgery or Medical Interventions
– Procedures related to the prostate can impact penile tissue
– May cause damage to nerves or blood vessels
– Can lead to scar tissue development in certain cases
8. Lifestyle and Sexual Practices
Certain habits induce mechanical strain on the penis:
– Intense or forceful sexual activity
– Insufficient lubrication
– Ignoring discomfort during sex
– Repeated minor injuries over time
These practices heighten the risk of microtrauma.
9. Connective Tissue Disorders
– Conditions that impair collagen production heighten risk
– These disorders often lead the body to create excess scar tissue following injuries
Such conditions predispose individuals to abnormal healing responses.

Key Insight
Most men with Peyronie’s Disease have multiple risk factors, for instance:
– Age + diabetes
– Erectile dysfunction + recurrent injury
– Genetics + poor blood flow
An increased number of risk factors correlates with a greater chance of developing the condition.
Lifestyle and Behavioral Factors
Apart from medical and genetic influences, day-to-day habits can significantly affect the onset of Peyronie’s Disease. Many of these factors lead to repeated stress or trauma to the penis, elevating the risk of scar tissue formation over time.
1. Intense or Forceful Sexual Activity
– Abrupt or unrestrained movements during intercourse can create microtears in penile tissue
– Positions that apply excessive pressure or bending stress on the penis heighten the risk
– Ongoing strain hinders healing and results in plaque formation
2. Inadequate Lubrication
– Lack of sufficient lubrication raises friction during sex
– Increased friction equates to a greater chance of tissue irritation and injury
– Over time, this may lead to inflammation and scar tissue generation
3. Disregarding Pain or Discomfort
– Experiencing pain during erection or sex serves as an early warning signal
– Engaging in sexual activity despite pain can exacerbate tissue damage
– Putting off attention allows the issue to worsen
4. Inactive Lifestyle
– Low levels of physical activity diminish blood circulation
– Restricted blood flow impacts tissue repair and healing
– Boosts the risk of inflammation and fibrosis
5. Smoking and Excessive Alcohol Use
– Smoking harms blood vessels and cuts down oxygen availability
– Alcohol misuse can disrupt hormonal balance and healing
– Both factors promote chronic inflammation and hinder recovery
6. Poor Nutrition and Diet Deficiencies
– Diets lacking essential nutrients and antioxidants slow the healing process
– High processed food intake heightens inflammation
– A deficiency in nutrients (like Vitamins E and C) can hinder tissue repair
7. Unregulated Use of Sexual Enhancers
– Unregulated substances can provoke prolonged or forced erections
– Increased rigidity without control heightens injury risk
– Some enhancers may negatively impact blood flow
8. Repetitive Mechanical Stress
– Frequent bending or pressure on the penis (intentional or accidental)
– Certain habits or activities that continuously strain the penile tissue
– Over time, this contributes to chronic microtrauma
READ ALSO: Top 7 Best Medicines To Last Longer In Bed
Key Takeaway
Lifestyle decisions significantly influence your risk of Peyronie’s Disease. Many of these issues are preventable, making awareness and behavioral changes a crucial method for protection.
Medical Conditions Associated with Peyronie’s Disease
Several underlying health issues are closely connected with Peyronie’s Disease development. These conditions often influence blood vessels, connective tissue, or the body’s healing response, making scar tissue formation more probable after even minor injuries.
1. Connective Tissue Disorders
– Disorders impairing collagen production raise the risk of abnormal scar formation
– Dupuytren’s contracture is a well-known associated condition
– Both conditions manifest excess fibrous tissue accumulation
Men affected by these disorders are more susceptible to plaque development in the penis.
2. Diabetes
– Elevated blood sugar levels damage small blood vessels
– Decreases oxygen supply to penile tissue
– Slows the healing process and fosters fibrosis (scar tissue formation)
Diabetes remains one of the strongest medical risk factors.
3. Erectile Dysfunction (ED)
– Weak erections result in diminished penile rigidity
– Raises the likelihood of bending or injury during sex
– Chronic ED can lead to reduced blood flow and compromised tissue health
ED and Peyronie’s Disease frequently exacerbate each other.
4. Cardiovascular Disease
– Encompasses heart disease, atherosclerosis, and poor circulation
– Restricts blood flow vital for tissue repair
– Contributes to chronic inflammation and vascular impairment
Healthy blood vessels are crucial for preventing plaque formation.
READ ALSO: 7 Best Treatments for Stroke: Effective Options For Recovery And Prevention
5. High Blood Pressure (Hypertension)
– Gradually harms arteries
– Diminishes elasticity and blood flow
– Impedes the body’s natural healing processes
This creates an environment prone to scar tissue development.
6. Autoimmune Disorders
– The immune system may erroneously target healthy tissue
– Provokes chronic inflammation throughout the body
– May lead to abnormal healing and scar tissue
Though less common, autoimmune responses may clarify cases without clear injury.
7. Prostate-Related Conditions and Surgeries
– Procedures like prostate surgery can impact nearby nerves and blood vessels
– May result in tissue trauma or decreased blood supply
– In some cases, this triggers scar development
Key Insight
These medical conditions do not independently cause Peyronie’s Disease. Instead, they:
– Weaken tissue integrity
– Diminish blood flow
– Disrupt normal healing
This renders the penis more susceptible to plaque formation following injury.

Can Peyronie’s Disease Develop Without Injury?
Yes—Peyronie’s Disease may arise even in the absence of a clear penile injury. While trauma and microtrauma are common contributors, many men report no identifiable incident prior to symptoms arising. This complexity adds layers to the condition than typically assumed.
1. Subtle or Undetected Microtrauma
In numerous instances, the “injury” is not overt or noticeable.
– Small tissue tears may happen during ordinary sexual activity
– These injuries could go without immediate pain or visible harm
– Over time, repeated, unnoticed trauma leads to scar tissue accumulation
Thus, even in the absence of a significant event, damage can build gradually.
2. Abnormal Wound Healing Response
Some individuals have unique healing processes.
– Instead of seamless tissue repair, the body may create excess collagen
– This results in thick, rigid scar tissue (plaque)
– Plaque can manifest without a clearly identifiable cause
This explains how Peyronie’s Disease can emerge unexpectedly for some.
3. Genetic and Biological Influences
Genetic predispositions can affect internal body responses.
– Some individuals are more prone to fibrosis (excessive scar formation)
– A family history of connective tissue disorders raises risk
– The body may excessively react to standard tissue stress
This accounts for why two men leading similar lifestyles can experience vastly different outcomes.
4. Silent Inflammation
Inflammation doesn’t always manifest as pain.
– Low-grade inflammation can develop within the penile tissue
– This may slowly harm tissue structure over time
– Eventually, scar tissue emerges even without a documented injury
5. Circulatory and Vascular Problems
Poor blood flow can facilitate disease progression.
– A reduced oxygen supply disrupts tissue repair
– Impaired blood vessels may render the penis more vulnerable
– This increases the chances of internal structural changes
6. Metabolic and Health Conditions
Certain medical issues amplify risk even in the absence of trauma:
– Diabetes
– High blood pressure
– Chronic cardiovascular illness
These conditions interfere with normal healing and tissue upkeep.
Key Takeaway
Peyronie’s Disease can arise even without a discernible injury due to a combination of:
– Hidden micro-injuries
– Unusual healing responses
– Genetic predispositions
– Poor vascular health or underlying medical issues
This highlights the importance of early awareness; even men lacking evident risk events can still develop the condition.

Frequently Asked Questions (FAQ)
1. Can Peyronie’s Disease resolve on its own?
While Peyronie’s Disease may show slight improvement in some men during the initial (acute) stage, in most cases, the condition does not fully resolve without intervention. Once scar tissue (plaque) forms and stabilizes, the curvature typically persists unless addressed through medical or therapeutic means.
• 2. Is Peyronie’s Disease a serious condition?
• While it is not life-threatening, it can profoundly impact one’s quality of life. The disorder may lead to:
• Painful erections
• Challenges during sexual intercourse
• Emotional anxiety or diminished self-esteem
• Erectile dysfunction in some instances
Early detection is crucial for preventing progression and complications.
3. Can younger individuals develop Peyronie’s Disease?
Yes. Although it is primarily observed in men over 40, younger individuals can also experience it. In these cases, it is often associated with:
• Sports-related or sexual trauma
• Genetic factors
• Abnormal healing responses
4. Does Peyronie’s Disease inevitably worsen over time?
Not necessarily. The condition usually progresses through two stages:
• Acute phase: Pain and changing curvature
• Chronic phase: Stable curvature with reduced or absent pain
For some men, the condition stabilizes without severe progression, while others may experience deterioration if left untreated.
5. Is Peyronie’s Disease linked to masturbation?
There is no solid evidence to suggest that masturbation alone causes the condition. However, intense or rough sexual activities (including masturbation) that result in repeated micro-injury may play a contributing role over time.
6. Does Peyronie’s Disease impact fertility or sexual performance?
It does not have a direct effect on sperm production or fertility, but it can:
• Make sexual intercourse challenging or painful
• Diminish the quality of erections
• Influence sexual satisfaction and confidence
Conclusion
Peyronie’s Disease arises from a combination of physical injuries, biological reactions, lifestyle choices, and existing health issues. While trauma—both significant and minor—serves as a major catalyst, many men develop the condition due to genetics, aging, diabetes, poor circulation, and atypical wound healing.
The key takeaway is the importance of early awareness. Identifying risk factors and initial signs can significantly enhance management outcomes and prevent worsening curvature. Even when no specific injury is recalled, internal mechanisms such as microtrauma and excessive collagen development can still result in plaque formation.
By maintaining overall health, managing chronic conditions, and avoiding repetitive penile strain, men can lower their risk and safeguard long-term sexual well-being.